Hepatitis C
What is Hepatitis C ?
Hepatitis C is a liver disease caused by the hepatitis C virus, or HCV. Many people infected with the hepatitis C virus develop a chronic infection because their body’s immune system is unable to remove the infection.
You can have hepatitis C for many years with no symptoms. Many people are infected with the virus and do not even know it.
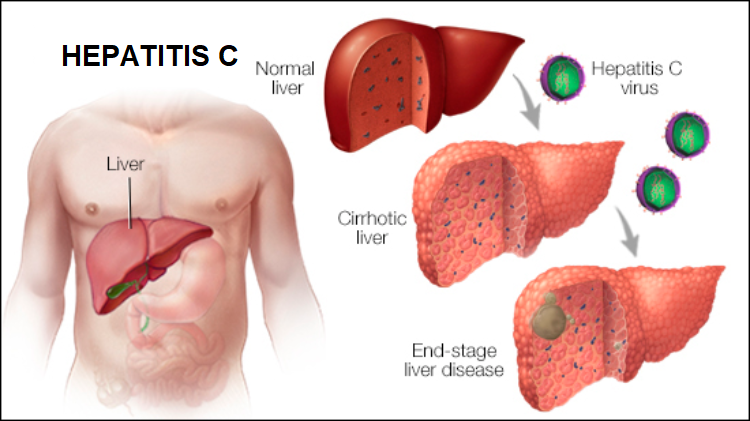
Symptoms and how the disease progresses vary from person to person. Many people do not develop serious health problems and have normal blood tests, no symptoms and little or no liver damage. Others develop a condition called cirrhosis, liver failure or liver cancer.
Read this information to help you understand hepatitis C, and how it is diagnosed and treated. Talk to your health care provider if you have questions or concerns
Understanding liver :
Knowing how your liver works normally helps you understand hepatitis C. The liver is the largest solid organ in your body. It is in the upper right part of your abdomen under your ribs. The liver makes substances you need to live and it inactivates harmful ones.
Liver functions include:
- Making proteins.
- Processing drugs.
- Removing waste products.
- Making bile for digestion.
Good liver function is needed for normal digestion and nutrition, muscle building, blood clotting and storage of nutrients. Everything you eat, drink, breathe and absorb through your skin eventually reaches your liver. For you to be healthy, you need a healthy liver.
What are the risk factors for getting Hepatitis C ?
People born between 1945 and 1965 have the highest risk of having hepatitis C. This generation has been called “baby boomers.” If you did get HCV during that time, you may not even know it. If you were born during this time, talk with your provider about being tested for HCV.
Risk factors include having:
- Received a blood transfusion, blood product or organ transplant before 1992.
- Injected street drugs, even for only a short time.
- Hemodialysis for kidney disease.
- Another liver disease such as hepatitis B.
- Been born to a mother who has hepatitis C.
- Had sexual contact with someone who has hepatitis C.
- Had sexual contact with someone who has a history of sexually transmitted diseases.
- HIV.
- Gotten a tattoo or a body piercing in an unsterile environment.
- Used non-injected street drugs such as those you swallow by mouth, smoke or inhale.
- A shared toothbrush, nail clipper or razor.
If you have any of the risk factors listed here, see your provider and get tested.
How does Chronic Hepatitis C spread ?
Hepatitis C is spread through exposure to infected blood or body fluids including through:
Sharing needles or instruments for illicit drug use. Hepatitis C can be spread through contaminated needles, inhaled cocaine use or other instruments used for drugs.
Blood transfusion. Currently, hepatitis C is almost never transmitted by blood transfusions. However, before 1992, when dependable blood screening tests for hepatitis C virus became available, people were infected with the virus through blood transfusions.
Sexual contact. Hepatitis C can be transmitted sexually but it is rarely passed through one sexual encounter. Transmission is also rare in a long-term relationship with one partner.
However, your risk for getting hepatitis C goes up if you practice high-risk sexual behaviours such as having multiple sexual partners. If you do have multiple partners, use latex condoms and have regular medical check-ups. If you have hepatitis C, tell your sexual partner and encourage him or her to be tested for hepatitis C.
Childbirth. Babies born to women with hepatitis C have a small increased risk of getting the disease. Half the babies who acquire the disease from their mother do not remain infected because their bodies resolve the infection on their own. There is no evidence the virus is spread through breast-feeding.
Accidental needle pricks. The risk of health care workers getting hepatitis C from an accidental needle prick from any patient is less than 1 percent. If the patient has hepatitis C, the chance is 5 to 10 percent. The spread of hepatitis C from health care workers to patients is very rare.
Hepatitis C infection is NOT spread by:
- Close contact such as hugging and kissing.
- Sneezing or coughing.
- Sharing eating utensils or drinking glasses.
- Food or water.
- Casual contact such as brushing by someone in a crowded hallway.
Since there is no vaccine for hepatitis C, the only way to prevent it is to avoid becoming infected and to take steps to prevent giving it to others.
If you have been diagnosed with hepatitis C, follow these guidelines to prevent the spread of hepatitis C:
- Do not donate blood, tissue, body organs or semen.
- Do not get body piercings and tattoos.
- Do not share needles.
- If you have multiple sexual partners, use condoms.
- Tell your sexual partners that they should be tested for hepatitis C.
- Do not share toothbrushes, nail clippers, razors or manicure scissors with others.
- Cover open sores or any breaks in the skin until completely healed.
If you have questions about a specific activity or how hepatitis C is spread, ask your health care provider.
How Hepatitis C Progresses ?
Hepatitis C usually progresses slowly over years. The disease may stay in a mild state, or it may advance, causing serious liver damage.
Phase 1.Infection occurs when the hepatitis C virus enters the bloodstream andbegins to infect the liver cells. Your body’s immune system usually is not successful in getting rid of the hepatitis C infection. About 75 to 85 percent of people who become infected with the hepatitis C virus stay infected. During this early phase, very few people have symptoms, usually nothing more than feeling tired.
Phase 2.Liver inflammation happens when the immune system tries to get rid ofinfected liver cells. At this point, the disease has become chronic hepatitis, that is, it is long term. For some, liver inflammation is mild while for others, it is severe. People who have little or no liver inflammation may never progress to severe liver damage.
Phase 3.Fibrosis is the formation of scar tissue in the liver. Chemicals released in theliver during liver inflammation may stimulate certain liver cells to make scar tissue. Generally, if test results show you have significant fibrosis, you have had hepatitis C for more than 10 years.
The next part of this phase is cirrhosis. This is when the scarring has become widespread in a “honeycomb” pattern. Cirrhosis may affect how your liver works. Progressive fibrosis can lead to increased pressure needed for blood to flow through the liver, called portal hypertension. About 20 to 30 percent of people with hepatitis C develop cirrhosis. The longer you have hepatitis C, the greater your chance of developing cirrhosis. Other risk factors that increase the risk of cirrhosis are:
- Moderate-to-heavy alcohol consumption.
- Being a man.
- Being over age 40 at the time of becoming infected with hepatitis C.
Phase 4. End-stage liver disease many happen if you have cirrhosis for a longtime. End- stage liver disease can lead to liver failure and increased pressure in the abdominal veins, called portal hypertension. Another complication of liver disease is primary liver cancer, called hepatocellular carcinoma. If you have cirrhosis, your risk of developing liver cancer is 3 to 4 percent each year. People who develop liver cancer have usually had hepatitis C for 30 years or more.
What are the symptoms of Chronic Hepatitis C ?
Most people who have hepatitis C have no symptoms in the early phases.
If symptoms happen, they usually begin about 8 weeks from the time you were first infected and they are similar to flu symptoms which may include:
- Upset stomach.
- Feeling very tired.
- Poor appetite.
- Headaches.
- Right upper abdominal pain.
- Muscle or joint pain.
Someone with chronic hepatitis C may have no symptoms until the disease is advanced. Abnormal yellow colour of the skin and eyes, called jaundice, may be the first symptom of chronic hepatitis C.
Other symptoms may include:
- Dark urine.
- Gray, light-coloured, black or bloody stools.
- Throwing up blood.
- Abdominal swelling, called ascites.
- Long-term itching.
- Feeling weak.
- Mild-to-severe mental confusion.
- Excessive bruising.
- Frequent nose bleeds.
If you have symptoms of hepatitis C, see your health care provider right away.
How is Chronic Hepatitis C diagnosed ?
Health care providers can use many tests to diagnosis hepatitis C, but none of the tests are part of a routine physical. If you have any of the risk factors, tell your health care provider.
Diagnosis may include:
Blood tests
Exposure to hepatitis C virus can be detected by a simple blood test called an HCV antibody test. When you are exposed to an infection, your body produces antibodies. If you are exposed to hepatitis C, your body produces the “anti-HCV” antibody and this shows up in the blood test.
Other blood tests include:
Liver enzymes
Tests for indicators of liver damage including ALT (alanineaminotransferase), AST (aspartate aminotransferase), and alkaline phosphatase.
Liver function tests
Tests for albumin, bilirubin and prothrombin time.
HCV RNA tests
Tests for the HCV virus and for how much of the virus is in yoursystem. This test may be repeated many times during treatment to see how well you are responding.
Genotyping
Genotyping is done to determine the specific strain (genotype) of HCV.
- There are six main genotypes (subtypes) of hepatitis C virus, numbered 1 to 6.
- Type 1 is the most common in the United States, found in about 65 to 75 percent of people while genotype 3 is most common in India
- Types 2 and 3 are easiest to treat.
Genotyping results can be used to determine how long you might need treatment and which treatment might be most effective for you.
If tests for hepatitis C are positive, your health care provider may order imaging exams of your liver.
Ultrasound is an imaging technique that uses sound waves above the hearing rangeto “see” organs. An ultrasound is used to look at the size, shape, texture and blood supply of the liver.
CT scans (computed tomography) are a type of X-ray that takes cross-sectionalpictures of the body. A CT scan is sometimes used to get a different view of the liver from that seen on ultrasound exams. Sometimes the CT scan can “see” something the ultrasound does not, or vice versa.
MRI (magnetic resonance imaging) scans uses the special properties of magneticfields and the atoms inside your body to create images.
MRE (magnetic resonance elastography) tests the elasticity of the liver using magnetic resonance imaging and low-frequency mechanical vibration. This test might be used instead of a liver biopsy.
A liver biopsy is a procedure in which a small piece of tissue is taken from the liver using a special needle. A liver biopsy is used to:
- Confirm the diagnosis of hepatitis C.
- Rule out other liver diseases.
- Allow your health care provider to assess the severity of your hepatitis C.
- Help your health care provider determine treatment.
- Help your health care provider to estimate the future course of your disease.
Using information from liver biopsies, health care providers describe the amount of liver scarring using a staging system, ranging from Stage 1 which is very little scarring to Stage 4 which is widespread scarring, or cirrhosis.
What is the treatment of Hepatitis C ?
Treatment for hepatitis C involves taking a combination of medications. This treatment is called “antiviral therapy.” The combination of medications you take depends on which specific strain, that is, genotype, of HCV you have. Before you begin treatment, you have a blood test done, called genotyping, to determine your specific strain. Other factors determine treatment as well such as the phase of the disease you are in, your symptoms and overall health.
Several new treatments are being developed to help treat and sometimes cure hepatitis C. The new treatments are not only proving to be more effective at treating the condition, but they also offer fewer side effects, are taken over a shorter length of time, and are available in a pill or tablet form that is easily taken by mouth.
Discuss available treatments with your health care provider. He or she determines what type of treatment will work best for you. Even if treatment in the past has not worked for you, a new treatment may. It is important to talk with your health care provider about all available treatments and which type of treatment may work best for you. You should also talk with your health insurance provider about coverage for treatment for hepatitis C.
Why treat hepatitis C? Some people wonder why their hepatitis C needs to be treated even though they are not having symptoms. Treating hepatitis C is like treating high blood pressure: it prevents greater problems down the road. You may not have had symptoms, but the hepatitis C virus may have been causing serious damage to your liver. Over time, this can lead to liver failure. This is why it is important that even though you may not have had symptoms, you should get treatment.
About Liver Transplants
Hepatitis C is the leading cause of permanent liver damage that requires a liver transplant. A liver transplant may be the only treatment option for people with liver failure. However, the likelihood that hepatitis C will lead to liver failure is small.
People with cirrhosis may develop liver failure. If you are diagnosed with cirrhosis, your physician will watch your symptoms and test results closely to determine whether your liver function is getting worse. After a diagnosis of cirrhosis is made, an upper endoscopy is typically used to look for varicose veins in the esophagus that can rupture and bleed. Liver cancer screening is advised for all anyone who has cirrhosis and should happen every 6 months with an ultrasound or other imaging test. If it seems like a liver transplant may be needed, your health care provider can make a timely referral. The timing of the referral is important because people needing transplants may be on the waiting list for one to two years before a liver becomes available.
Signs and symptoms that you have end-stage liver disease and may need a liver transplant include the following:
- Accumulation of fluid in the abdomen (ascites)
- Changes in mental function
- Gastrointestinal bleeding
- Jaundice
- Severe weakness
- Loss of muscle mass
Contact your health care provider if you have symptoms of liver failure that are not controlled by medication.
Is living with Hepatitis C possible ?
With new advances in treatment, you can live a normal life after having treatment. You can interact with your family as you always have. You can have close relationships. Women can become pregnant and breast-feed their babies.
Sometimes people who have hepatitis C do not need to have treatment and can live a normal life with the condition. Each person is different. Hepatitis C often takes many years before it affects the liver. And not everyone gets liver disease from the virus.
You may want to talk with your health care provider if you have questions about hepatitis C and your sexual relationship.
It is not necessary to change your eating habits as long as you eat a healthy, well-balanced diet. However, do not drink alcohol. Drinking alcohol increases the risk of liver damage.
Avoid medications that may damage your liver. Ask your health care provider about medications you take. If new medications are prescribed, tell your provider and pharmacist that you have hepatitis C. In general, small amounts of acetaminophen and other pain relievers are safe if you do not have advanced liver disease.
You can do your usual activities. In fact, it is a good idea to have some kind of regular exercise program. With the development of fibrosis, some people start to get increased pressure in the abdominal veins, called portal hypertension. If that is the case, mild aerobic activity such as walking, jogging, biking and swimming is better for you than activities that require straining such as heavy weightlifting. Ask your health care provider if weightlifting is appropriate for you.
Whatever exercise you do, pace yourself and rest when you feel tired.
How often you visit your health care provider depends on whether you are being treated for hepatitis C or have cirrhosis. Usually, people with hepatitis C see their health care provider about once a year.
If you do not have immunity to hepatitis A and B, get vaccinated. Talk to your health care provider about specific activities or concerns.
Remember
Finding out that you have a serious condition like hepatitis C can be hard. You might have many questions and feel overwhelmed by the amount of information you are receiving. First, remember that many people with hepatitis C lead full, productive lives. Second, remember that you do not have to manage alone. Your health care team is here to help.
If you have questions or concerns, talk with your health care team.




